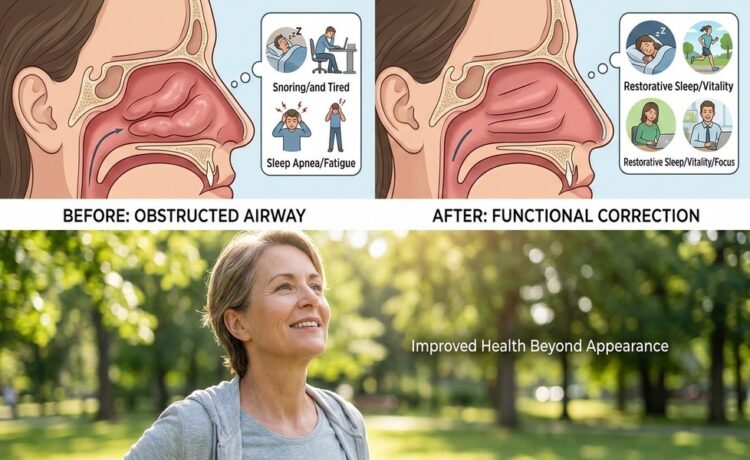
Nasal surgery is often talked about in terms of appearance, but many procedures are done for functional reasons. When the nose does not allow air to move properly, the effects can show up in everyday life. Exercise may feel harder, sleep may become restless, and routine activities can take more energy than they should.
Functional nasal surgery focuses on improving the structure and airflow of the nose. For some people, that means correcting a deviated septum. For others, it may involve repairing nasal valve collapse, reducing enlarged turbinates, or addressing damage from an injury. While the outside of the nose may change in some cases, the main goal is better breathing, better sleep, and improved daily comfort.
Understanding Functional Nasal Surgery
Functional nasal surgery is designed to correct physical problems inside or around the nose that interfere with normal airflow. Unlike purely cosmetic procedures, these surgeries focus on how the nose works. They look at how air enters the nose, how it moves through the nasal passages, and whether any structures are blocking that movement.
Common procedures include septoplasty, turbinate reduction, nasal valve repair, and functional rhinoplasty. These may be performed separately or together, depending on what is causing the breathing problem. Someone with a crooked septum may need a different approach than someone whose nasal sidewalls collapse during inhalation.
Some people seek care after years of adapting to poor breathing. They may not realize how much effort they use just to get enough air through the nose. Once the obstruction is identified, treatment can be planned around the specific structural issue instead of focusing only on the symptoms.
How Nasal Structure Affects Breathing
The nose does more than provide an entry point for air. It warms, filters, and humidifies air before it reaches the lungs. When the internal structure of the nose is blocked or narrowed, these functions may not work as well. A person may start breathing through the mouth more often, especially during sleep or physical activity.
A deviated septum is one of the most common structural causes of nasal blockage. The septum is the wall between the two nasal passages. When it is crooked or displaced, one or both sides of the nose may feel restricted.
Enlarged turbinates can also narrow the airway. Turbinates are small structures inside the nose that help regulate airflow and moisture. They can become swollen because of allergies, irritation, or chronic inflammation.
Functional rhinoplasty may be considered when the outer or inner framework of the nose contributes to poor airflow. For example, North Texas Facial Plastic Surgery provides care related to functional rhinoplasty surgery, with a focus on improving nasal function when structure affects breathing. In these cases, the goal is not simply to reshape the nose. It is to support the airway so breathing feels more open and stable.
Better Sleep Through Improved Airflow
Nasal obstruction can have a noticeable effect on sleep quality. When air does not pass easily through the nose, a person may wake up often, breathe through the mouth, snore, or feel unrefreshed in the morning. Even mild nasal blockage can make sleep less restful because the body has to work harder to maintain steady breathing.
Mouth breathing during sleep can also lead to dry mouth, sore throat, and morning discomfort. Some people wake up feeling congested even when they do not have a cold. Others may notice they sleep better on one side because one nasal passage feels more open than the other.
Functional nasal surgery does not treat every sleep problem, and it is not a replacement for a sleep apnea evaluation when one is needed. Still, improving nasal airflow may reduce nighttime breathing resistance. For some patients, this can make sleep feel deeper and less interrupted. It may also make treatments such as CPAP therapy more comfortable when nasal obstruction has made them difficult to use.
Daily Comfort and Physical Activity
Breathing problems can affect small parts of daily life in ways that are easy to overlook. Climbing stairs, walking outside, working out, or speaking for long periods may feel harder when nasal airflow is limited. Some people unconsciously shift to mouth breathing, which can feel less comfortable and less efficient.
During exercise, the body needs more oxygen. If the nasal passages are blocked, a person may feel winded sooner or struggle to maintain endurance. This does not always mean the lungs or heart are the main issue. Sometimes the nose itself is creating resistance before air reaches the lower airway.
Functional nasal procedures may help reduce that resistance. When the airway is more open, breathing can feel smoother during both rest and movement. This can improve comfort during workouts, outdoor activities, and routine tasks. The change may be subtle at first, but many people notice that breathing takes less conscious effort.
The Role of Sinus and Airway Evaluation
Not all breathing problems come from the same source. Some are structural, while others are related to sinus disease, inflammation, infection, or allergies. That is why a careful evaluation matters before deciding on surgery. A provider may examine the nasal passages, review symptoms, and use imaging or nasal endoscopy when needed.
For airway and sinus care, an ENT clinic in Plano, TX, may evaluate patients with chronic congestion, sinus pressure, recurring infections, or suspected nasal obstruction. This type of assessment can help distinguish between a fixed blockage and swelling that changes over time.
A full airway and sinus evaluation can also help prevent unnecessary treatment. For example, if congestion is mainly caused by uncontrolled inflammation, medical therapy may be recommended first. If there is a clear structural issue that does not improve with medication, surgery may become part of the discussion.
Allergies, Inflammation, and Nasal Breathing
Allergies can make nasal breathing much worse. When the immune system reacts to pollen, dust, mold, pet dander, or other triggers, the nasal lining can swell. This swelling narrows the airway and increases mucus production. For people who already have a deviated septum or narrow nasal passages, allergic inflammation can make obstruction feel more severe.
Allergy-related breathing issues may come and go depending on the season or environment. Someone may breathe fairly well during part of the year, then feel constantly congested during allergy season. Others may have year-round symptoms from indoor allergens. This can make it harder to know whether the main problem is structural, inflammatory, or both.
Because of this overlap, allergy management is often part of a broader breathing plan. West Hills Allergy & Asthma Associates addresses allergy-related breathing issues, which may include identifying triggers and helping reduce inflammation that affects the nose and airway. When allergies are better controlled, it may become clearer how much of the remaining obstruction is related to nasal structure.
Recovery and Realistic Expectations
Recovery from functional nasal surgery depends on the procedure performed. Some surgeries involve internal changes only, while others require adjustment of the nasal framework. Swelling, congestion, and mild discomfort are common early in the healing period. It may take weeks or months for the full breathing improvement to become noticeable.
Realistic expectations are important. Functional nasal surgery is intended to improve airflow, but results vary based on anatomy, healing, allergies, sinus health, and other medical factors. Some people experience a major improvement, while others notice a more gradual change. Follow-up care helps monitor healing and address concerns as the nose settles.
Patients are usually advised to avoid strenuous activity for a period of time after surgery. They may also need to use saline rinses, attend follow-up visits, and protect the nose from injury. Recovery is not just about waiting for swelling to go down. It also involves supporting the healing process so the airway can function as intended.
Whole-Body Health Considerations
Nasal breathing affects more than the nose itself. Poor nasal airflow can influence sleep, energy, exercise tolerance, and comfort throughout the day. When breathing feels restricted, people may compensate without realizing it. They may sleep poorly, avoid certain activities, or rely on mouth breathing as their default.
Ongoing health monitoring can be helpful, especially when symptoms overlap with other concerns. Fatigue, headaches, poor sleep, and reduced stamina can have many causes. A clinic focused on overall health monitoring, such as GrandForksClinic.com, may help patients track broader health patterns and decide whether nasal breathing is one part of a larger picture.
This broader view matters because nasal surgery is not always the only answer. Some people benefit from allergy care, sinus treatment, sleep evaluation, asthma management, or general medical follow-up. When these pieces are considered together, care can be more practical and better matched to the person’s needs.
When to Consider a Medical Evaluation
A medical evaluation may be appropriate when nasal breathing problems are persistent, one-sided, or interfering with sleep and daily life. Symptoms such as chronic congestion, frequent mouth breathing, snoring, recurring sinus infections, or difficulty breathing during exercise should not be ignored if they continue over time.
It is also worth seeking evaluation after nasal trauma. An injury can change the shape of the septum or weaken nasal support structures, even if the outside of the nose appears mostly normal. Some people notice breathing problems soon after an injury, while others develop symptoms gradually as swelling resolves or tissues heal in a narrowed position.
During an evaluation, a clinician may ask when symptoms started, whether they change with the seasons, and whether medications have helped. This information can guide the next steps. In some cases, medical treatment is enough. In others, functional nasal surgery may offer a more lasting solution for structural obstruction.
Final Thoughts
Functional nasal surgery can improve health in ways that go beyond appearance. By addressing structural problems that limit airflow, these procedures may support better breathing, more restful sleep, improved comfort during activity, and less strain in daily life.
The best approach starts with understanding the cause of the problem. Nasal obstruction may involve the septum, turbinates, nasal valves, allergies, sinus disease, or a combination of factors. A thoughtful evaluation can help determine whether surgery, medical care, or a combined plan is the right fit.
For people who have lived with restricted breathing for years, improved nasal function can make a meaningful difference. When the nose works more effectively, breathing often feels easier, sleep may improve, and daily routines can become more comfortable.